Explain the Process as You Work Through It
Different avenues and various support helped one client battle the aftereffects of a stroke.
In 1934, William Mixter and Joseph Barr published a groundbreaking study in the New England Journal of Medicine. It was the first study that made a strong correlation between intervertebral disc herniation and the symptoms of sciatica. It set off several decades of intense focus on addressing disc pathologies that were blamed for a vast array of low-back pain problems. This time period has frequently been referred to as the "Dynasty of the Disk," during which many surgeries were performed to address back and lower-leg pain. Unfortunately, what became painfully clear was that many people not only didn't improve from the surgeries, but a large number actually got worse.
In the latter part of the 20th century, advanced medical imaging technology allowed us to look at the disc with greater accuracy without invasive surgery. As a result, we now have a better understanding about the structure of the disc, factors that lead to degeneration and disc damage, and the role disc pathology may play in certain pain conditions. Interestingly, the more we have learned about spinal function and intervertebral disc structure, the more we have realized disc pathology is not a simple structural problem at all. In addition, we can no longer say with any certainty that simply because somebody has disc damage or herniation and corresponding pain, that the two are causally related. So, let's explore what we have learned about the disc and how this plays a role in many of the back and leg complaints clients bring to us.
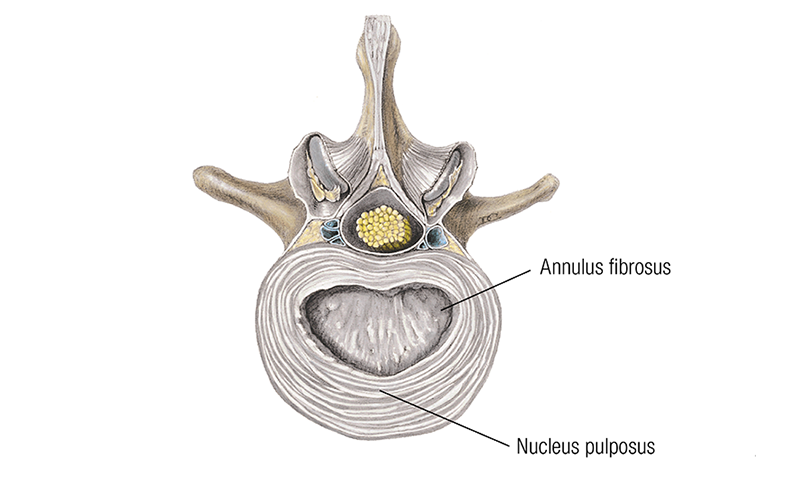
There are two primary components to the intervertebral disc. The gel-like structure in the center is called the nucleus pulposus. The softer nucleus is surrounded by concentric layers of fibrocartilage with fibers in alternating directions. These concentric layers of fibrocartilage make up the annulus fibrosus (Image 1). The alternating layers in the annulus give it both pliability and strength.
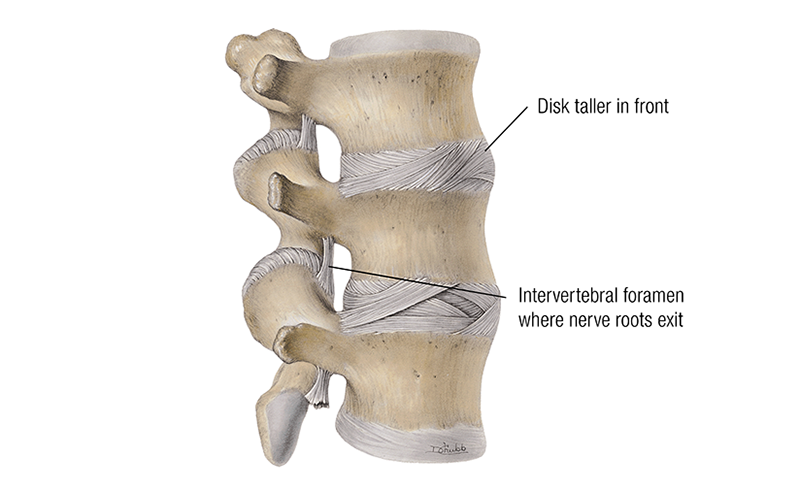
The primary function of the intervertebral disc is to manage the compressive loads of the spine during movements in multiple planes. The spine is curved to help manage and absorb some of these loads. Consequently, the disc shape has to accommodate the spinal curvature as well. So, in the lumbar region, where there is a natural lordotic curvature, the intervertebral disc is taller on the front side than the back (Image 2). If the spine loses its natural curvature, there are unequal forces on the disc and these long-term compressive loads lead to disc pathologies.
The intervertebral disc has fibers that are enmeshed into the body of each adjacent vertebra. This helps maintain structural integrity between the disc and the vertebra. Realizing that there are fibers deeply embedded between the disc and the body of the vertebra helps debunk a common image that goes along with the layperson's term of a "slipped disc." In most cases, the disc does not actually slip (except in the instance of a condition called spondylolisthesis mentioned later under "Disc Pathologies"). Instead, compressive loads may cause the disc to change shape or bulge out in a particular direction. This pathological process is described in the pages that follow.
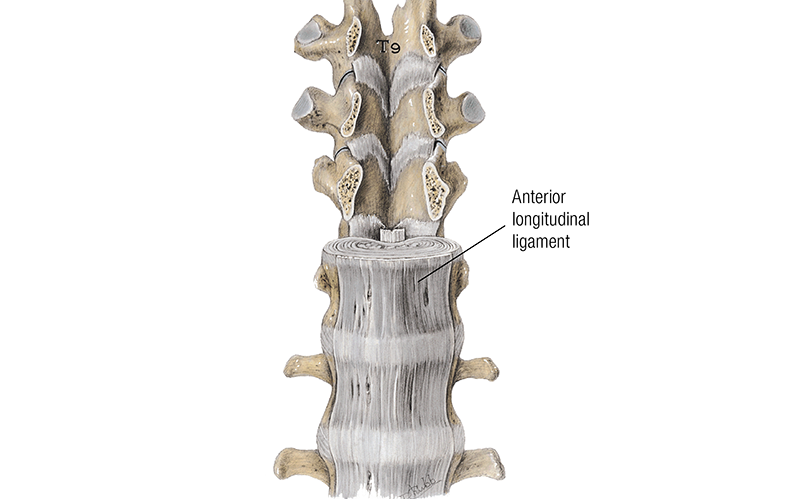
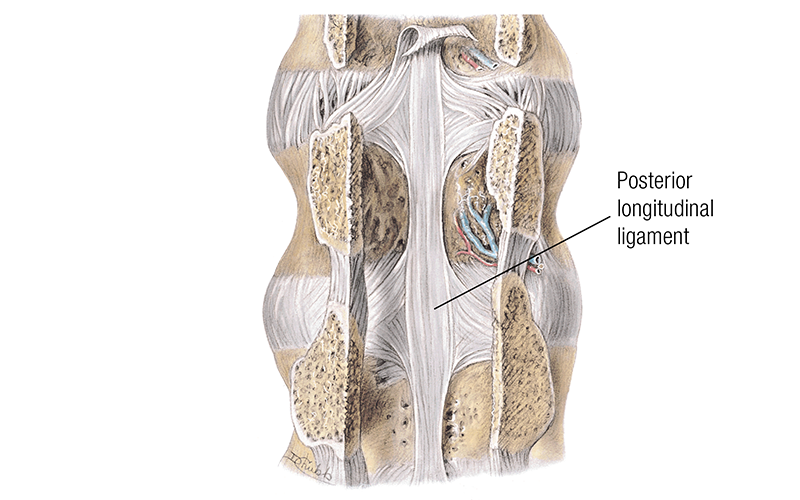
Another important factor about disc structure is its relationship to adjacent tissues. There is a long and broad ligament on the anterior aspect of the spine called the anterior longitudinal ligament (ALL). The ligament helps maintain the position and integrity of intervertebral discs throughout the spine (Image 3). There is a corresponding ligament on the posterior side of the lumbar vertebra called the posterior longitudinal ligament (PLL), and it spans the length of the spine inside the spinal canal (Image 4). However, it is much narrower than the ALL and, therefore, limits the restraining capability of this ligament on the posterior side, which plays an important role in disc pathologies as well. Immediately adjacent to the PLL is the spinal cord, and the ligament is an important restraint to keep disc bulges from pressing on the spinal cord.
Immediately adjacent to the posterior lateral aspect of the disc are the nerve roots that exit the spinal cord and pass through the intervertebral foramen (Image 2). This is the location where these nerve roots are vulnerable to compression by deforming discs.
Multiple terms describe damage and dysfunction to the intervertebral discs. Recently, there have been concerted efforts to improve this terminology challenge with standardized terms and concepts defining disc pathologies.1 Massage therapists may encounter these terms in clients who have seen other health professionals, and it is valuable to understand these terms so we have a good understanding of our role in addressing the client's complaint.
There are three main categories of disc pathology: annular tears, disc degeneration, and disc herniations. Let's explore the definition and physiology of each variation to better understand what is occurring with spinal structures and the impact on local and distant pain conditions.
An annular tear (also called an annular fissure) involves a disruption or separation between fibers of the annulus fibrosus. It may also occur when the annulus pulls away from one of the adjacent vertebral bodies (called an avulsion). Annular tearing and avulsion from the vertebral body is partly what occurs in a condition called spondylolisthesis, where the disc does actually move or migrate across the top of the vertebral body.
There is no way to identify annular tears through any type of physical examination; these are determined with high-tech diagnostic imaging. Because annular tears frequently don't change the shape of the disc, they may not press on adjacent structures and cause any significant symptoms.
The next category of disc pathology is called degeneration. Degeneration results from a variety of sources that may include multiple annular tears, loss of water content in the disc, disintegration of the annulus, and vertebral osteophytes. Degeneration usually involves a loss of disc thickness, which then causes spinal stenosis.
Spinal stenosis involves a narrowing of the intervertebral foramen caused by the vertebrae coming closer together. The intervertebral foramen is a small opening where nerve roots exit the spine. When the foramen is reduced, there is a greater likelihood of nerve root compression.
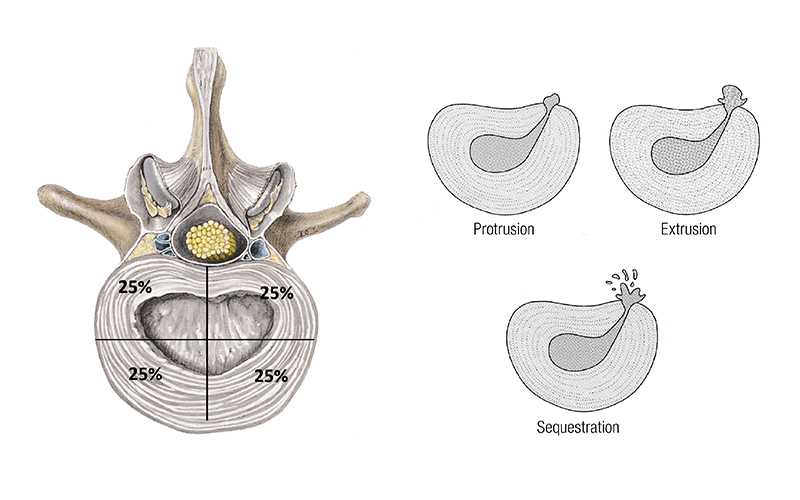
The third category of disc pathology is called herniation. Disc herniation is the pathology most associated with low-back or cervical pain or pain that extends down the length of the extremity from affected nerve roots. What is sometimes confusing about disc herniations are the various terms used to describe different types of disc pathology. The herniation is defined as a "localized displacement of disc material beyond the limits of the intervertebral disc space."2
There are several types of disc herniations, and the easiest way to understand them is with a diagram that describes the percentage of disc displacement (Image 5). If there is a displacement that affects more than 25 percent of the disc, it is considered a broad-based displacement and generally referred to as a disc bulge. Most disc bulges are the result of annular tears. If the displacement involves 25 percent or less of the disc, it is generally referred to as a focal herniation. Focal herniations are then broken down into two separate categories:
In some cases, disc material from extrusion will continue to separate from the main body of the disc. This is called a sequestration.
When material in the nucleus pushes out the edge of the annulus and causes a disc herniation, the primary concern is that disc material can press on adjacent structures, particularly nerve roots. Herniations most commonly occur at the posterior lateral edge of the disc, as there is no restraint by adjacent tissues in this direction. Unfortunately, this is where the nerve roots are located.
Massage therapy cannot change the amount of disc herniation, but it can play a very helpful role in managing some of the neurological sensations that perpetuate pain problems.
In some cases, the disc will push straight posteriorly against the posterior longitudinal ligament. When it does, there is a good chance it will press directly on the spinal cord. This occurs most frequently in the lumbar region and can be a dangerous situation called cauda equina syndrome. Symptoms of this syndrome indicate nerve compression on both motor and sensory fibers of the spinal cord and include low-back or lower extremity pain; bowel, bladder, or sexual dysfunction; or other symptoms of pelvic floor sensory or motor impairment. If your client is exhibiting any of these symptoms, especially if they are felt bilaterally, they should immediately consult a physician.
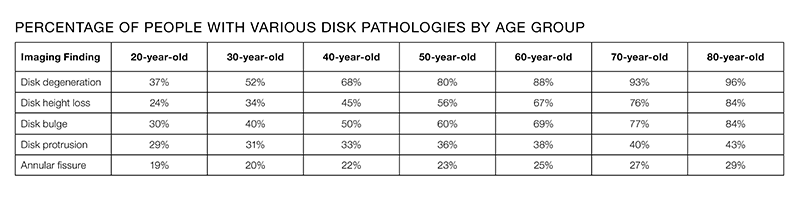
One of the things we have learned from recent MRI studies is that disc pathology happens in a high percentage of the population who have no symptoms whatsoever. The table below shows a comparison chart of the frequency with which various disc pathologies exist in healthy individuals with no symptoms. That means just because somebody has a herniated disc, even if they have corresponding pain, we can't determine that their pain is necessarily coming from the disc problem. Some studies have also shown that people's pain perceptions can possibly increase after being shown medical imaging (such as MRI or X-ray) that indicates apparent damage or dysfunction.
The table shows various age brackets and the percentage of people in that bracket with imaging who show disc pathology (but not necessarily any pain or symptoms).3
Identifying disc pathology with physical examination is challenging. Various physical examination methods, such as the straight leg raise test or slump test, are used in conjunction with clinical signs to suggest the likelihood of disc pathology. However, high-tech diagnostic studies, such as MRI, are needed to confirm the presence or severity of disc pathology.
What is important for massage therapists to consider is what role our treatments can play in addressing various disc pathologies. Because we now realize that asymptomatic people can have disc herniations, it is likely you work on people with these conditions without even knowing it. However, it is important to recognize that sometimes disc pathology is a primary part of someone's pain complaint, and we want to make sure we don't exaggerate their pain with inappropriate soft-tissue treatment.
Back or neck pain can come from a wide variety of sources. A disc pathology is one possibility, but just because it exists, it doesn't mean it is the sole source of their pain. Massage therapy cannot change the amount of disc herniation, but it can play a very helpful role in managing some of the neurological sensations that perpetuate pain problems. If a client presents with relevant symptoms or a diagnosis of disc pathology, use caution in treating the area and be particularly attentive to avoiding anything that increases symptoms.
Massage therapists are sometimes wary of working on people who have disc herniations because of a fear of pressing directly on the location of nerve root compression. Keep in mind that the most common locations for nerve root compression are anterior to the transverse processes of the spine, and we cannot actually press on those areas.
Another interesting factor about disc pathology is that recent research has shown that many disc pathologies involving herniations can spontaneously regress and symptoms be resolved simply through time and appropriately protected movement. If you can reduce the offending activities and noxious pain sensations, it is possible that spontaneous regression of the disc and pain resolution may occur in some cases.
A potential benefit of massage treatment is that working on affected muscles in the area of a disc herniation may help reduce compressive loads exacerbated by hypertonic muscles. This, in turn, can decrease overall muscle tightness and compressive loads even further. The soothing sensations that massage produces also decrease discomfort and help in pain management. The importance and value of the pain reduction massage produces should not be underestimated when addressing the symptoms of disc pathology.
The best guideline is to use gentle and soothing techniques, whatever they may be, that help encourage relaxation and ease in the area without being too invasive. These strategies can help a wide variety of disc pathologies, and your client will be very thankful for the strategies you have used to help them manage their life and get out of pain.
1. David F. Fardon et al., "Lumbar Disk Nomenclature: Recommendations of the Combined Task Forces of the North American Spine Society, American Society of Spine Radiology and the American Society of Neuroradiology," Spine Journal 14, no. 11 (2014), https://doi.org/10.1016/j.spinee.2014.04.022.
2. W. Brinjikji et al., "Systematic Literature Review of Imaging Features of Spinal Degeneration in Asymptomatic Populations," American Journal of Neuroradiology 36, no. 4 (2015): 811-16. https://doi.org/10.3174/ajnr.A4173.
3. W. Brinjikji et al., "Systematic Literature Review of Imaging Features of Spinal Degeneration in Asymptomatic Populations."
Different avenues and various support helped one client battle the aftereffects of a stroke.
Caring for elderly clients requires the massage therapist to have a keen awareness, not only of the characteristics unique to the client but also of the various members of the client’s care team.
This variation of your massage stance can reduce discomfort, help conserve strength, and use your movement and body weight most efficiently during a session.
When focusing on stretching a target muscle, sometimes other muscles in the group need to be considered for the session to be effective.