Explain the Process as You Work Through It
Different avenues and various support helped one client battle the aftereffects of a stroke.
Forward-head posture has become the defining musculoskeletal pattern of modern life, and we see it every day in our sessions. Hours spent focusing on small visual targets such as phones, laptops, and tablets shift the cranium anteriorly relative to the thorax, altering load distribution throughout the entire kinetic chain. While many of us use techniques that reduce tension in the muscles of the cervical region and upper thoracic spine, we can do more to address joint restrictions with manual therapy.
Let’s examine the biomechanics of the spine and teach several methods that improve cervical joint mobility.
The cervical spine is the most mobile and neurologically sensitive region of the vertebral column (Image 1). Its structure reflects a dynamic balance between stability, mobility, and sensory regulation.
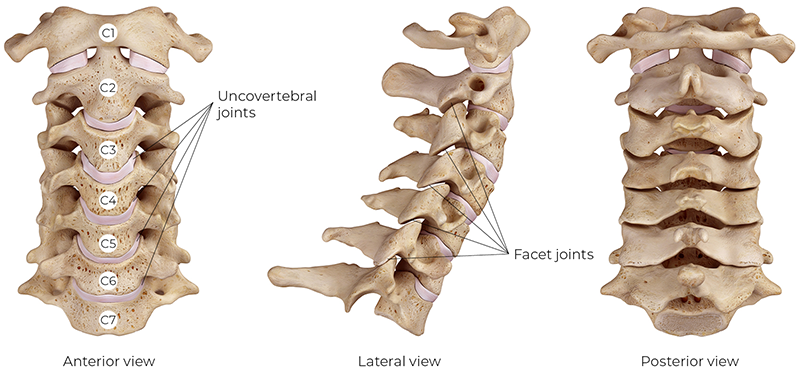
The atlanto-occipital (AO) joint formed between the occipital condyles of the skull and the superior articular facets (lateral masses) of the atlas (C1) accounts for approximately 50 percent of cervical flexion and extension. This is the same motion of your head nodding yes.
The AO joint plays a primary role in maintaining a horizontal visual field, which is essential for balance and spatial orientation. Forward-head posture alters AO joint mechanics, forcing the joint and related muscles to work harder to keep the head level. Restrictions here can contribute to eye strain, dizziness, and cervicogenic headaches and may influence shoulder and thoracic positioning.
The atlantoaxial (AA) joint is a complex of three separate articulations between the atlas and axis (C1 to C2). Two lateral articulations occur between the inferior articular facets of C1 and the superior articular facets of C2. The third articulation is the anterior arch of C1 and the odontoid process (dens) of C2, held in place by the transverse ligament. Research demonstrates that 50–60 percent of all cervical rotation occurs at the AA joint.
Understanding the layered biomechanics of the cervical spine clarifies why forward-head posture produces cervical joint restrictions and widespread dysfunction.
Dysfunction at the AA joint is the primary source of cervicogenic headaches caused by both hyper and hypomobility. Hypermobility results when the transverse and alar ligaments are relaxed. The neuromuscular system detects the instability and responds by splinting the area with the suboccipital muscles and cervical stabilizers (longus colli, longus capitis, rectus capitis anterior and lateralis, semispinalis cervicis, multifidus, rotatores, interspinales, and intertransversarii).
Hypomobility results from tightening of the alar ligament in response to a lack of movement in the AA joint (C1–C2) or C2–C3, fibrotic degenerative changes to joint capsules, and muscle guarding, especially of the suboccipital muscles. Interestingly, hypermobility can present as hypomobility because muscle guarding is so
intense that the joint appears fixated.
The transition from the highly specialized C1 to C2 complex to the more typical facet-joint architecture of C2 to C3 represents a major mechanical shift in the cervical spine. C2 to C3 must disperse rotational load from above while simultaneously managing flexion-extension and lateral flexion forces coming from below. This concentrated stress amplifies shear and compressive forces on the facet joints. Additionally, the AO and AA joints are often restricted in forward-head postures, so C2 to C3 compensates with excessive rotation, overloading the facet joint surfaces and leading to irritation. The deep cervical extensors and rotatores muscles splint the area with protective guarding.
The C2–C3 facet joint is innervated by the third occipital nerve, a branch of the dorsal ramus of C3. This nerve has direct referral patterns into the suboccipital, temporal, and mastoid regions, the upper trapezius, and behind the ear. Facet dysfunction at C2 to C3 contributes to cervicogenic headaches.
The C3 to C7 segments of the cervical spine share a consistent structure involving intervertebral discs, uncovertebral joints, and paired facet joints angled at approximately 45 degrees to the horizontal plane. The lower cervical segments rely on coupled motion, understood as the predictable way in which two or more movements occur together at the same spinal segment due to the shape of their facet joints, intervertebral discs, and ligamentous constraints. In the cervical spine, this means that rotation and sidebending always happen simultaneously in the same direction.
For example, when a client sidebends their head to the right, the lower cervical vertebrae will also rotate slightly to the right. Likewise, directing the head into right rotation inherently creates a small amount of right sidebending. This automatic pairing ensures smooth facet gliding, maintains joint stability, and prevents shearing forces that would occur if the motions happened independently.
Forward-head posture significantly alters mechanics in this region. As the head drifts anteriorly, the lower cervical spine is pulled into chronic flexion, increasing disc pressure and placing tensile load on the posterior ligaments. To maintain a horizontal gaze, the deep neck extensors and the upper trapezius contract, increasing muscle tone around the lower cervical facets. Over time, the combined effects of shear, compression, and ligamentous tension can reduce intervertebral foraminal space, sensitize facet joint capsules, and contribute to mechanical irritation of the nerve roots.
The uncovertebral joints are unique to the cervical spine between the C3 and C7 vertebrae. They are formed by the uncinate processes of the vertebrae below interlocking with the vertebral bodies above, facilitating flexion and extension while limiting lateral flexion and rotation. Forward-head postures increase shear and compressive forces on the uncovertebral joints, leading to degenerative changes that can cause arthritis, bone spurs, and reduced foraminal space, contributing to nerve root irritation, radiculopathy, and headache pain.
Understanding the layered biomechanics of the cervical spine clarifies why forward-head posture produces cervical joint restrictions and widespread dysfunction. Because these patterns are interconnected, the approach by Myoskeletal Alignment Techniques (MAT) is holistic and focused on methods that level the head, reduce muscle guarding, and enhance pain-free movement.
Following are six essential techniques for the cervical spine that can help make a difference for clients when integrated with your current methods.
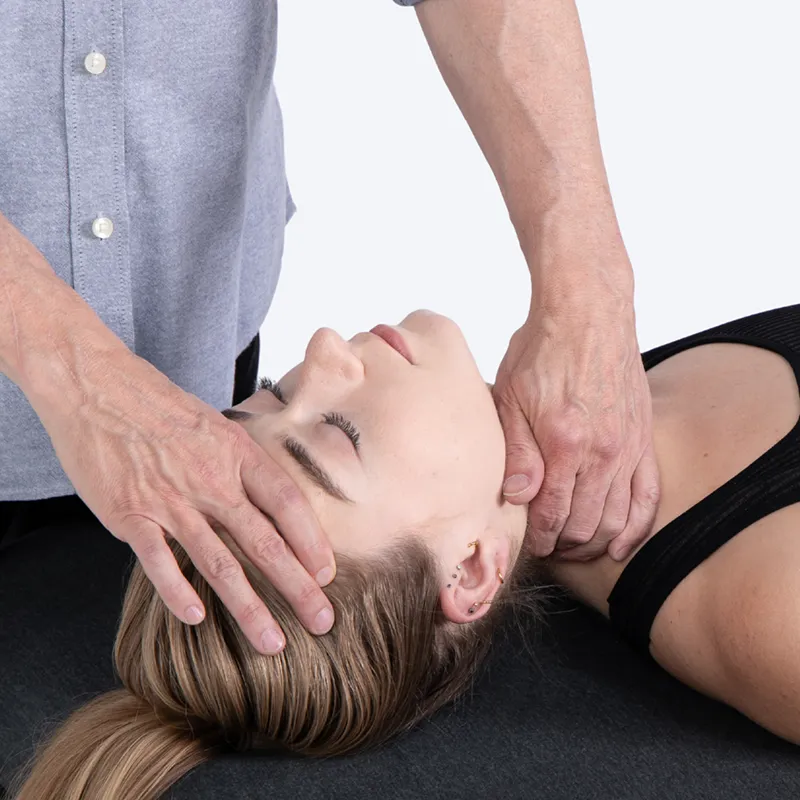
This technique warms the cervical soft tissue. First, stand on the client’s left with your right hand on the client’s forehead and your left hand draped over and around the client’s lateral neck. Establish a counterforce with your left hand (and extended arm) as it gently pulls the client’s neck anteriorly. At the same time, your right hand resists the client’s left head rotation. As you continue this rhythmic maneuver, curl your fingers to hook the suboccipitals and pull them anteriorly to work across their fibers. Repeat this stretch on the opposite side.

Place the flat palm of your nondominant hand under the back of your dominant hand and lift the client’s head and neck so that your wrists rest on the table. Bring your thumbs a half inch apart and place them into the lamina groove on either side of the spinous processes. Mobilize the client’s neck by pushing up with both thumbs into the groove. The rhythmic action juts the client’s chin as each vertebral segment extends over the thumb fulcrum. Jut the client’s chin for two minutes.
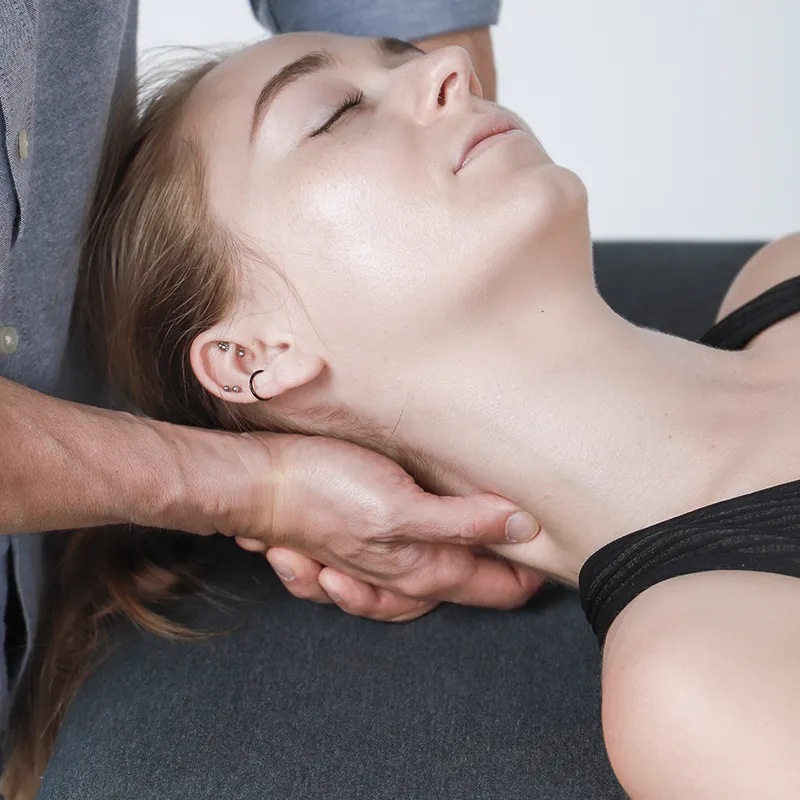
Your cupped palms support the client’s head as both of your thumbs pin lateral to the C5 spinous processes. Right sidebend the client’s neck with the right thumb pressing against the side of the spinous processes. Sidebend the client’s neck to the left with the left thumb pressing against the side of the spinous processes. Perform this technique bilaterally, working rhythmically from C2 to T1 and back again.
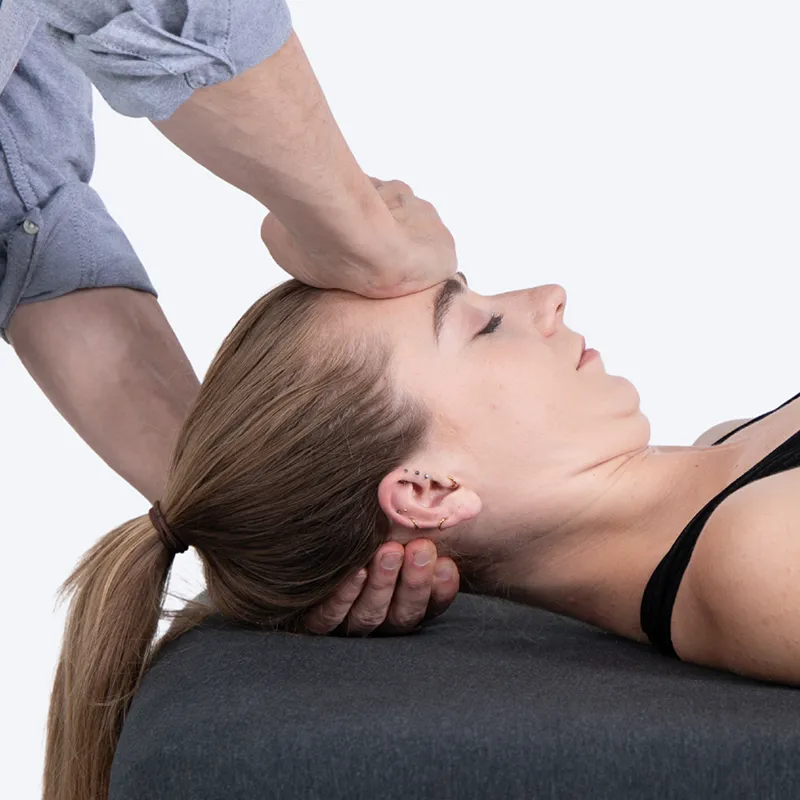
This procedure mobilizes the AO joint and stretches the suboccipitals. Standing at the head of the therapy table, slide your left hand under the client’s head to cradle it. Use your right hand to brace the client’s forehead. Ask the client to tuck their chin to their chest. With your elbows extended and your hands fixed, step to your right foot and apply a gentle two-second overpressure that places a stretch on the suboccipitals and encourages the occipital condyles to glide posteriorly. Work within the client’s comfort zone and repeat the chin tuck 3–4 times. Reverse your hand position, step onto your left foot, and repeat the technique 3–4 times.

The intertransversarii muscles extend between adjacent transverse processes, beginning at C1 (although the muscle between C1 and C2 is often absent) and continuing to T1. Each ventral ramus of the cervical region leaves its spinal nerve of origin and exits the spine by passing posterior to the vertebral artery and then between the anterior and posterior intertransversarii muscles. This intertransversarii stretch relieves nerve root, trunk, and cord compression of the brachial plexus.
Stand at the head of the table. Grasp and slowly rotate the client’s head left to its restrictive barrier. Gently lift the client’s head and neck to its first flexion barrier. Ask the client to inhale to a count of five and gently extend the head back toward the table against the therapist’s resistance. Slowly and gently lift the rotated head to the next flexion barrier as the client exhales. Repeat this stretch five times, then rotate the client’s head to the right and repeat the procedure. Notice that minimal effort is needed to stretch these small muscles. Use caution during rotation and flexion efforts. Discontinue this stretch if the client reports discomfort.

Grasp the client’s neck with both hands and lean back to gently decompress the neck, upper trapezius, and the sternocleidomastoid. Repeat the techniques shown in Images 4 and 5 up to five times.
Different avenues and various support helped one client battle the aftereffects of a stroke.
Caring for elderly clients requires the massage therapist to have a keen awareness, not only of the characteristics unique to the client but also of the various members of the client’s care team.
This variation of your massage stance can reduce discomfort, help conserve strength, and use your movement and body weight most efficiently during a session.
When focusing on stretching a target muscle, sometimes other muscles in the group need to be considered for the session to be effective.